IOL Services - Dysphotopsia (glare/haloes)
Background
Dysphotopsia is a disturbance of vision and includes light phenomena such as haloes; the subjective perception of a bright ring around a light source.1 Haloes may lead to disability glare, which is defined as the subjective perception of a significant loss in retinal image contrast due to an inappropriate distribution of light sources.1 The resultant loss in contrast, due to light scattering, typically reduces the observer's ability to distinguish detail within a visual scene. The corresponding glare may also cause discomfort, distracting the individual.
Uses
Quantification of light scatter can differentiate between different simultaneous vision, multifocal intraocular lens (IOL) designs and has been used as an objective measure of optical performance and patient satisfaction.2,3
Conventional tests
There are various pictorial representation charts, subjective questionnaires and psychophysical techniques (e.g., using the C-Quant device - Oculus Inc., Wetzlar, Germany), which attempt to quantify the amount and type of light scatter experienced by an individual. Measurements of halo size can be achieved with a Glare & Halo program (Tomey; Nagoya, Japan).2,3 However, this method is entirely subjective and relies on the patient to self-identify the outline of their perceived haloes (along 12 meridians), which may generate variable results. In addition, the C-Quant device does not appear to differentiate between light scatter for eyes implanted with multifocal and monofocal IOLs.4,5
Our approach
We are currently developing a novel method of quantifying halation that removes a significant proportion of the patient's subjective input. This technique involves identification of randomised letter targets – presented circumferentially around a glare source – to outline any perceived haloes (Figure 1). Early results have demonstrated high repeatability and successful differentiation between rotationally symmetric and sectorial multifocal IOLs (Figure 2).6

Figure 1. The Aston Halometer test displayed on a portable laptop PC
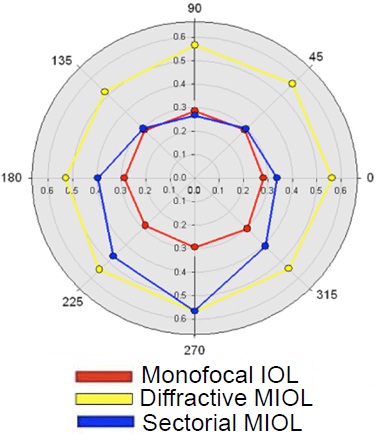
Figure 2. The angular position and size of photopic scotomas induced by different IOL designs (MIOL = Multifocal IOL)
References
- Aslam TM, Haider D & Murray IJ. Principles of disability glare measurement: an ophthalmological perspective. Acta ophthalmologica Scandinavica. 2007;85:354-60.
- Dick HB, Krummenauer F, Schwenn O, Krist R & Pfeiffer N. Objective and subjective evaluation of photic phenomena after monofocal and multifocal intraocular lens implantation. Ophthalmology. 1999;106:1878-86.
- Pieh S, Lackner B, Hanselmayer G, et al. Halo size under distance and near conditions in refractive multifocal intraocular lenses. Br J Ophthalmol. 2001;85:816-21.
- Cervino A, Hosking SL, Montes-Mico R & Alio JL. Retinal straylight in patients with monofocal and multifocal intraocular lenses. J Cataract Refract Surg. 2008;34:441-6.
- Hofmann T, Zuberbuhler B, Cervino A, Montes-Mico R & Haefliger E. Retinal straylight and complaint scores 18 months after implantation of the AcrySof monofocal and ReSTOR diffractive intraocular lenses. J Refract Surg. 2009;25:485-92.
- Buckhurst PJ, Wolffsohn JS, Shah S, Naroo S & Davies LN. Evaluation of Dysphotopsia with Multifocal Intraocular Lenses. Invest Ophthalmol Vis Sci. 2011;52:(E-Abstract 6185).
